If you are thinking about getting pregnant, it’s best to cover all the bases and get as much help as possible to make it happen. With the rising infertility rates, pre-existing conditions and a list of myriad things causing stress, conceiving can become a difficult process. While desi nuskhe from your nani, dadi, maa might seem like they can help, nothing beats professional medical guidance.
In conversation with TC46, Reproductive Medicine Specialist Dr Apurva Satish Amarnath, of Nova IVF Fertility, Bangalore shares 10 things couples can adopt to increase their chances of getting pregnant and having a healthy baby.
1. Ultrasound, blood tests and tubal function tests determine a woman’s chances of getting pregnant

Female evaluation includes an ultrasound, blood tests for ovarian reserve and checking of tubal function.
Ultrasound Examination
This is usually done on Day 2 or 3 of the cycle, to check the ovary for the number of follicles (antral follicular count), and the presence of any cysts, and to check the uterus for its cavity, fibroids, and endometrial polyps. Normal tubes are usually not seen on ultrasound. Pathological tubes, such as hydrosalpinx are imaged. All this helps evaluate if there are any issues that will impede pregnancy.
Blood Tests For Ovarian Reserve
This is usually done on Day 2/3 of the cycle. This includes FSH, LH, E2 and AMH – this lets us know what the overall pool of eggs in the ovaries is, and what the probability of conception is.
X-ray Imaging
An X-ray of the womb and fallopian tubes after a special dye has been inserted is called a hysterosalpingogram. It can be used to locate blockages in your fallopian tubes, which could be preventing eggs from making their way into your womb.
Laparoscopy
This is a technique that allows doctors to see through the body. A small cut in your lower tummy is made to allow a thin tube with a camera at the end (a laparoscope) to be inserted to examine your womb, fallopian tubes, and ovaries during laparoscopy (keyhole surgery).To highlight any blockages in your fallopian tubes, a dye can be injected into them through your cervix.
2. Men need to undergo semen analysis tests along with hormone analysis and ultrasounds

The main test for men is a semen analysis – this enables us to analyze the sperm and check for the concentration motility and morphology of the sperm. This is done to look for sperm issues like a low sperm count or sperm that aren’t moving properly. Additional tests such as hormone analysis and ultrasound is done – to further assess the cause of problems.
3. Ultrasounds to track the follicle (egg) are vital
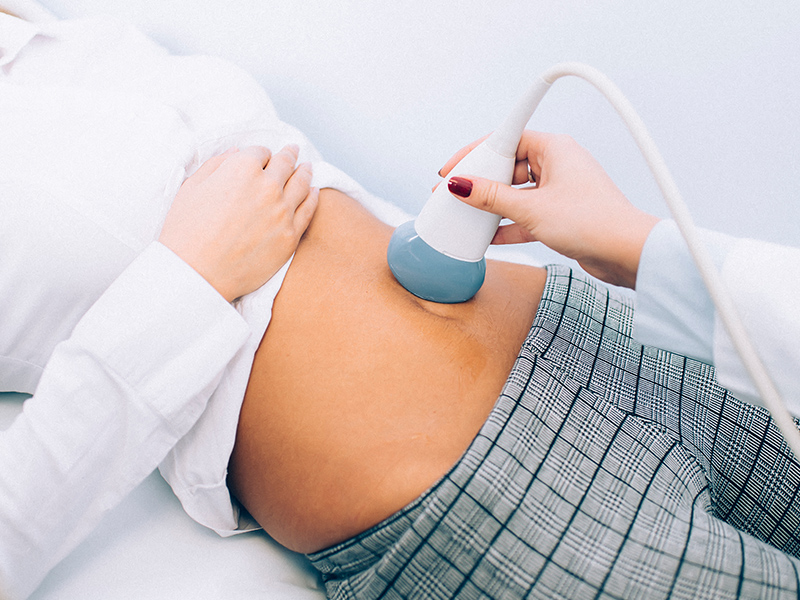
Menstruation refers to the shedding of the uterine lining during a woman’s monthly cycle. Estrogen and progesterone levels are low. The interval between the first day of your period and ovulation is known as the follicular phase. As an egg prepares to be released, oestrogen levels increase. The proliferative phase occurs after the cycle when the uterine lining regenerates. Ovulation is the mid-cycle release of the egg from the ovary. Estrogen peaks right before the event and then decreases quickly. The luteal phase is when the body prepares for a potential pregnancy between ovulation and the start of menstruation. Progesterone is made, peaks, and then gradually decreases. The secretory process occurs when the uterine lining releases chemicals that either support an early pregnancy or prepare the lining to break down and shed if pregnancy does not occur.
So some of the things that are tracked every cycle is how the follicle (egg) is growing, the corresponding endometrial thickness and evidence of ovulation – this is done usually with an ultrasound.
4. You are the most fertile 12 to 14 days before your next cycle

When you ovulate (when an egg is released from your ovaries), which typically happens 12 to 14 days before your next cycle, you’re at your most fertile. This is the most likely time of the month for you to become pregnant. It’s important to remember this applies to regular cycles between 26-32 days. If you have irregular cycles, then it’s very likely that you aren’t ovulating and should meet a fertility specialist to find the causes and treat the same.
5. An hCG level of more than 25 mIU/mL is considered positive

The hormone used to detect pregnancy is BHCG. This is detected in 2 ways – the most common is the urine pregnancy test – which is the home pregnancy test commonly used for pregnancy detection. It shows up as 2 lines to determine pregnancy. The other method of detection is using a blood test to detect the BHCG. The blood test gives us The standard hCG levels differ dramatically from one woman to the next. This is because hCG levels are highly dependent on your personal norms, how your body reacts to pregnancy, and the number of embryos you’re carrying. A woman’s body responds to pregnancy in a completely different way than a man’s.
An hCG level of less than 5 mIU/mL is considered negative for pregnancy, whereas a level of more than 25 mIU/mL is considered positive. If your hCG level is between 6 and 24 mIU/mL, you’ll probably need to be retested to see if your levels increase to confirm a pregnancy. The blood test gives more information and helps in identifying the fate of the pregnancy at times.
6. Prenatal supplements and folic acid should be taken
Take a vitamin and mineral supplement that contains at least 0.4 milligrams of folic acid (400 micrograms). Folic acid lowers the risk of birth defects, especially problems with the spine of the infant. Before you try to conceive, start taking a folic acid-rich vitamin. The needs to be started prior to pregnancy by at least a month. In women who are diabetic, epileptic on medication and have a previous history of neural tube defects need to take a higher dose of folic acid – 5mg daily 1 month prior to pregnancy and continued 3 months after.
7. Whatever the sex positions may be, the sperm moves up the female genital tract in 30 seconds

There is no particular position for sex that improves the possibility of pregnancy. Irrespective of position, the sperm moves up the female genital tract in 30 seconds. So do what makes you feel comfortable and let nature take its course.
8. The AMH test helps determine a woman’s capacity to produce fertile eggs for pregnancy
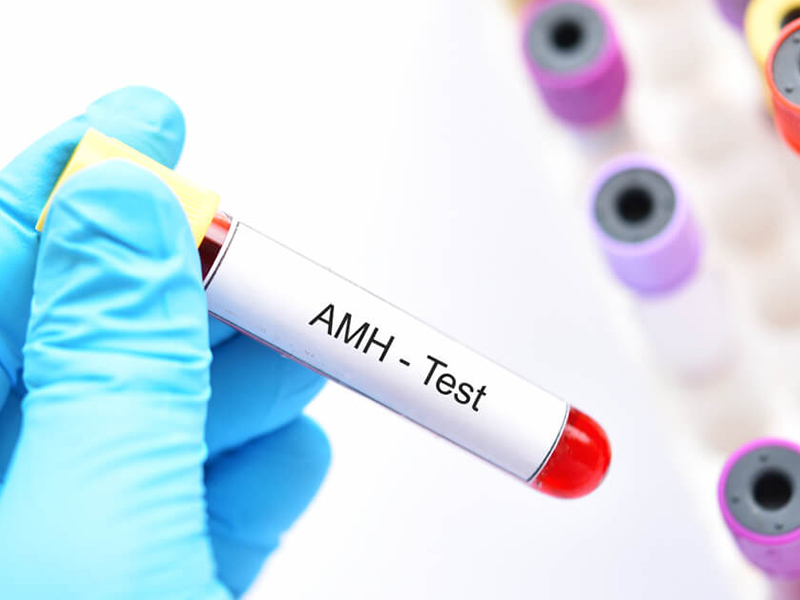
The amount of AMH in a woman’s blood may indicate how many potential egg cells she still has. The ovarian reserve is the term for this. An AMH which is low indicated a poorer chance of pregnancy – IVF may be required to expedite the process. A high AMH indicated the possibility of PCOS. A normal reserve shows that the chances of pregnancy are good. It must be remembered that AMH is not the sole marker of ovarian reserve and it always needs to be interpreted in relation to age since an increase in age causes a decline in both the number and quality of eggs and egg quality is an important marker of future pregnancy capability.
9. Age and lifestyle choices are the determinants of the quality of eggs
Theoretically only one egg and one sperm are required for pregnancy to happen. But usually, the number is discussed In relation to IVF. It is seen that 15 eggs are required for the possibility of healthy live birth and the number required increases with increasing age. The most important determinant of the quality of the egg is the age and associated lifestyle factors such as obesity, and smoking. The presence of other conditions such as endometriosis further depletes egg quality. There is no way to determine the quality of an egg. The only way to tell whether an egg is chromosomally normal is to try to fertilise it and then conduct a genetic test on the resulting embryo.
10. One of the best and least invasive fertility therapies is ovulation induction if you think your fertility chances are impaired
Start with your fertility specialist, she will give you pre-conception advice and tests, and if you’ve been trying for 1 year and haven’t had any luck.
Your doctor will even give you advice on how to make the necessary lifestyle changes, as well as help you figure out which days of the month you are most fertile, so you have the best chance of becoming pregnant.
One of the best and least invasive fertility therapies is ovulation induction. It entails taking medication to encourage eggs to mature in the ovaries and be released, thus raising the chances of becoming pregnant by timed intercourse or artificial insemination. Ovulation induction is best for women who produce low levels of ovulation hormones or who do not ovulate at all but have regular fallopian tubes and have no fertility issues with their male partner.
In vitro fertilisation (IVF) and intrauterine insemination (IUI) are two widely used fertility treatments. Artificial insemination, also known as intrauterine insemination, entails passing a male’s sperm via the cervix and into the uterus near ovulation. It is a less invasive and less complicated method of fertility treatment. IVF (In Vitro Fertilization) is a procedure in which a woman’s eggs are fertilised with a man’s sperm outside of the body and then transplanted back into the woman’s body.
Embryos that can be frozen. A frozen embryo transfer is a procedure in which a frozen embryo from a previous fresh IVF cycle is thawed and transferred back into the uterus of a woman. It means the woman won’t have to go through another round of hormone stimulation, and egg collection frozen embryo cycles can be done on your regular cycle or with the help of ovulation induction.
Other options include the use of egg donor, sperm donor or surrogacy where medically indicated.


