Psoriasis is a lot more stigmatised than most other skin diseases. Most people avoid physical contact with patients of psoriasis because they (incorrectly) assume the condition is contagious. What’s more, the chronic skin condition causes physical pain, discomfort, and can be emotionally challenging because of its highly visible nature.
Every year, August is recognised as Psoriasis Awareness Month, and this year we’ve roped in Dr Prashant Dash, Chief Medical Director at DocOnline Health, to share invaluable advice, treatment options and home remedies for psoriasis.
1. What is psoriasis and how does it affect the body?
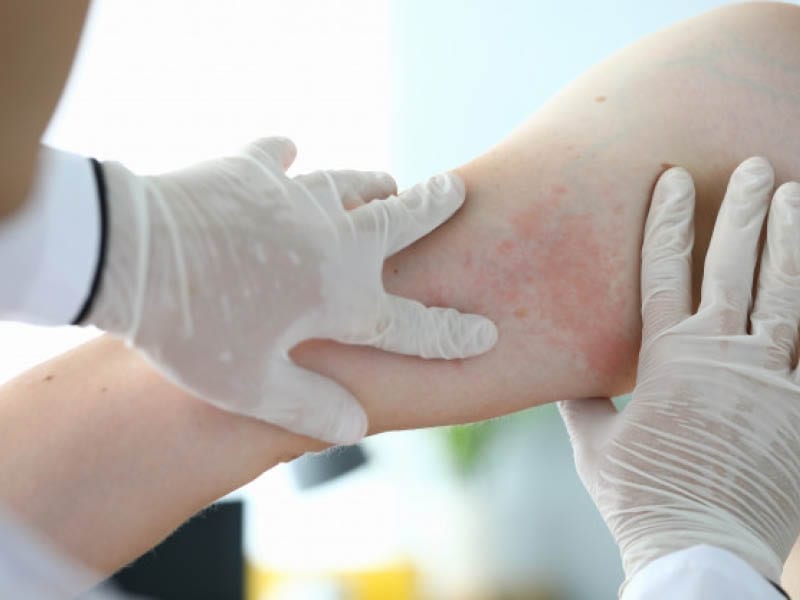
Psoriasis is a chronic inflammatory, non-contagious skin condition affecting approximately 125 million people worldwide.
It is typically lifelong, with a fluctuating course of exacerbations and remission of lesions, which may be aggravated by genetic, infectious, emotional, and environmental factors.
Psoriasis significantly impairs the quality of life of patients and their families, resulting in great physical, emotional and social burden.
2. How common is psoriasis among women? Do hormones play a role in the onset of psoriasis in women?

It is found to be slightly more common in males compared to females.
Research has demonstrated that female hormones, especially estrogen, significantly influence the onset and flare-ups of psoriasis. For example, many females experience the onset of psoriasis with puberty when there is a significant rise in female hormones. Psoriasis also tends to worsen around periods and during menopause. Pregnancy, on the other hand, has a calming effect on psoriasis.
3. What are the signs of psoriasis? How does it usually present?
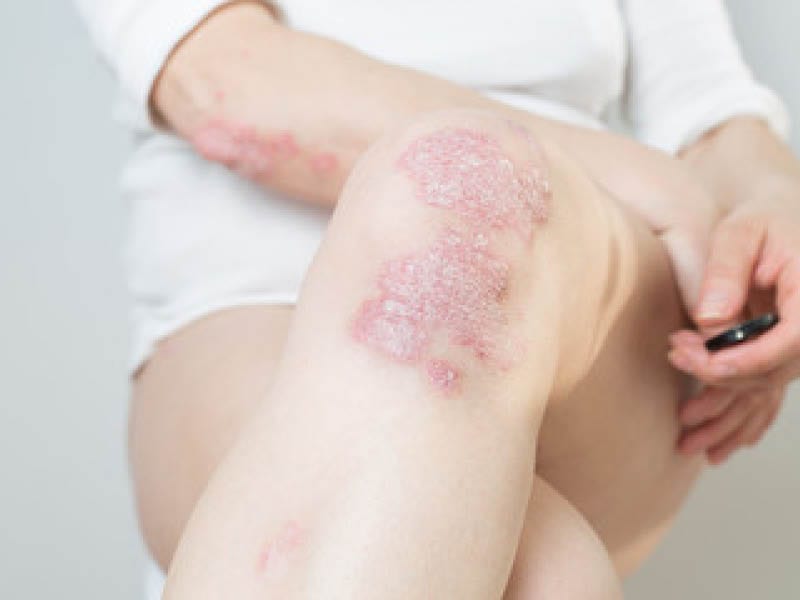
Psoriasis appears as red, thick, dry, itchy, silvery, scaly patches on the skin, commonly affecting elbows, knees, area in between buttocks and scalp. Signs and symptoms vary depending on the type of psoriasis and the severity of the disease. Some variants of psoriasis may involve the extremities (palms and soles), fingernails or the joints (psoriatic arthritis occurs in up to 15% to 30% of psoriasis patients).
4. What causes your psoriasis to flare-up?
The common causes of psoriasis flares are:
- Puberty or menopause: Women tend to experience worsening of symptoms before their periods, after delivery or during menopause due to fluctuations in levels of hormones, which influences the inflammation.
- Stress: Psychological stress aggravates the disease process, causing flare-ups. It affects the immune system and promotes the inflammatory response.
- Infections such as strep throat or a respiratory infection.
- Certain medicines like medication taken for high blood pressure, mental health disorders, antimalarials, and Indomethacin.
- Injury to skin like severe sunburns, bug bites, cuts or skin burns.
- Other factors such as smoking, alcohol, cold, dry weather, or being obese are known to worsen psoriasis.
5. At what age does psoriasis most commonly surface in women?
Psoriasis develops most commonly between the ages of 15 years to 35 years, but can be also seen in younger populations. Upto 10%-15% of patients get their first symptom before the age of 10 years.
6. What is the medical treatment for psoriasis?
| Severity | Treatment |
| Mild psoriasis | Topical creams and ointments (Steroid and/or retinoids creams) Skin moisturisers Shampoos (containing tar, salicylic acid) Home remedies |
| Moderate to Severe psoriasis | Combination treatments UV Light therapy + topical ointment UV Light therapy + Systemic therapy Systemic therapy (steroids, retinoids, methotrexate, cyclosporin) Biologics for severe cases who do not respond to the first line of treatment |
7. Are there any home remedies to soothe your skin if you’re experiencing a flare-up?
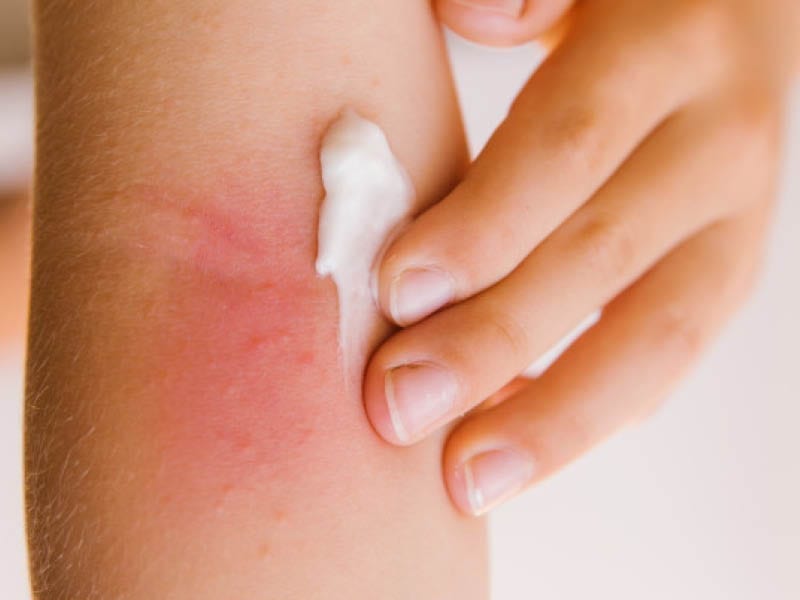
There are some steps which can reduce the psoriatic symptoms during a flare-up.
- Don’t scrub or rub skin during a shower; use a mild and gentle soap to avoid skin irritation.
- Moisturise your skin daily to prevent dryness. Apply a thick layer of petroleum jelly or moisturiser on the affected area so that water loss and redness is reduced.
- Stay in a comfortable and cool environment.
- Cover the area with a cotton cloth overnight to avoid scratching.
- Avoid triggers such as smoking, and alcohol.
- Exercise regularly and practise yoga and meditation to beat stress.
- Try salt (dead sea salt or Epsom salt) baths in warm water for at least 15 minutes and moisturise later.
- Eat less sugar and avoid consuming processed food. Have a low carb, high protein, balanced diet rich in fruits and vegetables to maintain healthy body weight to prevent obesity.
8. Is psoriasis genetic? If I have it, can I give it to my child?

Psoriasis is a hereditary disease but not all people carrying the defective gene manifest the disease. There are a lot of environmental factors that determine if a genetically susceptible person will develop psoriasis during their lifetime.
A parent, you have about a 10% chance of passing it down to your child. If both parents have psoriasis, there’s a 50% chance of passing down the disease.
9. Is psoriasis contagious?
No. Psoriasis is not contagious.
“Psoriasis isn’t contagious in any form. It’s an autoimmune condition — not an infectious disease.”
10. How do I know if it’s psoriasis and not some other skin condition like eczema, ringworm, and the like?
Psoriasis causes well-defined, thick, red, scaly patches, commonly in areas like the elbows and knees. It is common to see psoriasis on the face, buttocks, and scalp also. You’ll also see thick patches of skin with overlying redness.
Eczema presents as dry scaly patches and tends to appear in the crooks of the knees and the elbows. Itching is relatively much more in eczema than in psoriasis.
Ringworm causes a red, circular, and often scaly rash which is caused by a fungal infection (and not by a worm despite its name). It is also itchy and contagious.
These skin conditions may be very difficult to differentiate from each other. You need to always consult a doctor to aid in diagnosing and treating these skin conditions.